By Rebecca Morin, MLIS, MAS and Amy LaVertu, ML
If there is one thing everyone can agree on, it’s that the last few years have come with a lot of stress. While true for everyone, it is especially so for medical students, residents, fellows, and early career physicians. These groups experience higher levels of depression, burnout, depersonalization, and fatigue than peers outside of academic medicine [1]. Many are reluctant to seek help due to concerns regarding lasting stigma, exposure to peers and superiors, and lack of free time [2]. Even before the considerable pressure of the COVID-19 pandemic, it was clear that our patrons at the Tufts University Hirsh Health Sciences Library could benefit from programming focused on personal wellness and self-reflection.
Inspired to provide some relief to our medical students, my colleague Amy LaVertu and I set out to design a bibliotherapy program that would respect the unique challenges of medical school while measuring any benefit from participation. Bibliotherapy has many definitions, but we were guided by this one: “the basic premise of bibliotherapy is that information, guidance, and solace can be found through reading” [3]. Traditionally, bibliotherapy sessions function like book groups; everyone reading the same material and meeting regularly to discuss it, often guided by a clinical professional. To better suit our students, we crafted a modified bibliotherapy model. It would not require regular meetings, would preserve anonymity, and be administered entirely by librarians. We built in a large degree of freedom into the intervention, both in choice of readings and use of student time.
Shortly after this proposal was accepted for the 2020 MLA Research Training Institute, we were faced with the unprecedented challenge of teaching and supporting students through the frightening early days of the COVID-19 pandemic. Public interest in media related to plagues and pandemics helped provide a theme for the bibliotherapy study. It also built on the concept that consumption of tragic and horror narrative enables readers to better cope with fear and misfortune on a personal level [4]. We selected six excerpts (of which students would choose three), to serve as the bibliotherapy intervention. These excerpts are a blend of fiction and non-fiction. Publication dates ranged from 1665 to 2011, with estimated reading times of 11 to 32 minutes. Study participants were drawn from the Tufts University School of Medicine MD program. All students commencing studies in August 2020 were eligible; we recruited 30 students (15% of the class). We opted to construct this study as an interrupted time series, with subjects completing a wellness assessment for three months, then receiving the bibliotherapy intervention. This was followed by three more months of wellness assessment and a concluding focus group. We used the 10 Question Perceived Stress Scale (PSS-10) as our assessment instrument. Focus groups were conducted over Zoom.
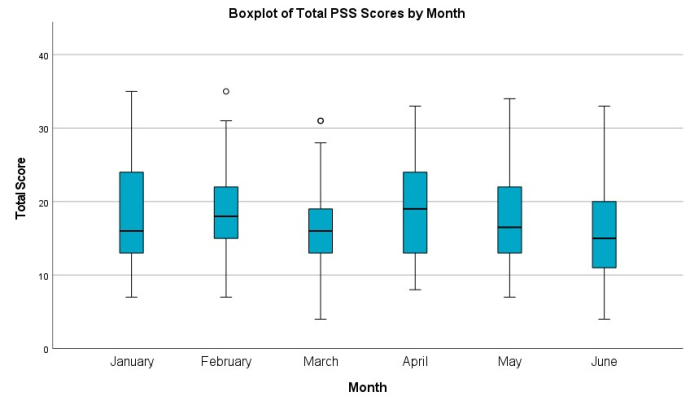
The study started in January 2021 and continued through July 2021. Subjects submitted one PSS-10 each month January-June, and completed the bibliotherapy intervention in March. The focus group series wrapped up in July. As we analyzed results of the monthly PSS-10 surveys, we did see a slight overall improvement post-intervention as compared to pre-intervention. This study, however, is not suitably powered to reveal any statistically significant findings. The focus groups revealed several common themes shared by the participants. Students reported feeling like their first year of medical school was a blur, with little time to reflect on one’s state of mind. They also reported acute feelings of isolation and struggling to meet new people and maintain relationships. Subjects noted that participation in the study helped them rediscover a love of reading outside of class. They wished we had provided opportunities to meet and discuss the readings as part of the intervention. Outside of the bibliotherapy intervention, many participants expressed gratitude for the monthly PSS-10, as it gave them a chance to regularly reflect upon their overall mental state. They also appreciated this initiative coming from the library, rather from their Deans and instructors.
The results of this study provide a foundation for building a more comprehensive bibliotherapy program at the Hirsh Health Sciences Library. We look forward to exploring this wellness modality with new groups of students.
References
- Dyrbye LN, West CP, Satele D, Boone S, Tan L, Sloan J, Shanafelt T D. Burnout among U.S. medical students, residents, and early career physicians relative to the general U.S. population. Acad Med. 2014; 89(3), 443-451. https://doi.org/10.1097/ACM.0000000000000134.
- Shahaf-Oren, B., Madan, I., & Henderson, C. (2021). "A lot of medical students, their biggest fear is failing at being seen to be a functional human": disclosure and help-seeking decisions by medical students with health problems. BMC Med Educ. 2021; 21(1), 599. https://doi.org/10.1186/s12909-021-03032-9.
- Brewster L, McNicol S, ProQuest. Bibliotherapy (1st ed.). 2018. Facet Publishing.
- Krieken K. How reading narratives can improve our fitness to survive: A Mental Simulation Model. Narrative Inquiry. 2018; 28(1), 139-160. https://doi.org/https://doi.org/10.1075/ni.17049.kri.